
Sleep apnea is a serious sleep disorder affecting millions worldwide, with 10% to 30% of adults experiencing this condition. It causes repeated interruptions in breathing during sleep, leading to loud snoring, gasping, and restless nights. Untreated, sleep apnea can lead to severe health risks like high blood pressure, heart disease, stroke, and diabetes.
Addressing sleep apnea is essential not just for improving sleep but for preventing these significant health complications. Fortunately, there are various effective treatment options available. These range from lifestyle changes and positive airway pressure devices to oral appliances and surgical interventions.
Each treatment is tailored to meet individual needs, ensuring better sleep and improved overall health. Whether it’s making lifestyle adjustments or using medical devices, the right approach can make a significant difference. Exploring these options is the first step towards a healthier life.
Positive Airway Pressure (PAP) Devices
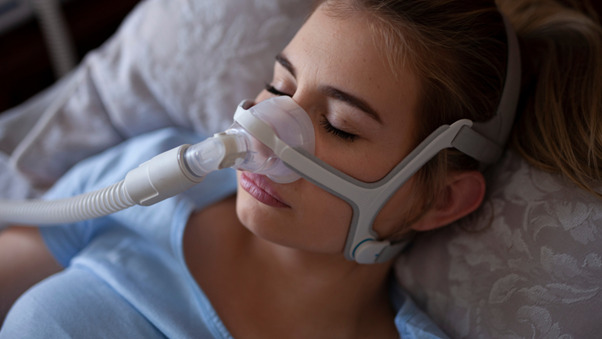
Continuous Positive Airway Pressure (CPAP)
Continuous Positive Airway Pressure (CPAP) is the leading treatment option for managing obstructive sleep apnea (OSA). It works by delivering a steady stream of air through a mask, keeping the airway open during sleep. While CPAP is highly effective, some patients may experience discomfort or noise, but newer models are quieter and offer various customization options like different mask styles, humidifiers, and adjustable pressure settings.
Auto-adjusting Positive Airway Pressure (APAP)
Auto-adjusting Positive Airway Pressure (APAP) devices differ from CPAP by automatically adjusting the air pressure based on your breathing patterns. This feature makes APAP ideal for individuals with variable pressure needs. It offers a more personalized treatment experience, adapting to your specific requirements throughout the night.
Bilevel Positive Airway Pressure (BiPAP)
Bilevel Positive Airway Pressure (BiPAP) is designed for patients who don’t respond well to CPAP. BiPAP provides higher pressure when you inhale and lower pressure when you exhale, making it more comfortable for certain users. This alternative is particularly useful for those who find CPAP difficult to tolerate.
Adaptive Servo-Ventilation (ASV)
Adaptive Servo-Ventilation (ASV) is used to treat both OSA and central sleep apnea (CSA). It automatically adjusts inhalation pressure based on your needs, providing targeted support. However, ASV is not recommended for individuals with specific heart conditions, so a thorough consultation with a healthcare provider is necessary to determine its suitability.
Oral Appliances
Mandibular Advancement Devices (MADs)
Mandibular Advancement Devices (MADs) are designed to treat obstructive sleep apnea (OSA) by moving the lower jaw forward. This forward movement helps keep the airway open during sleep, reducing the frequency and severity of apnea episodes. MADs are particularly effective for individuals with mild to moderate OSA and offer a less invasive alternative to continuous positive airway pressure (CPAP) therapy.
Tongue-Retaining Devices (TRDs)
Tongue-Retaining Devices (TRDs) work by holding the tongue in place to prevent it from blocking the airway during sleep. While less common than MADs, TRDs can be a useful option for patients who do not respond well to MADs. They are particularly helpful for those who experience tongue-related airway obstruction.
Importance of Consulting a Dentist
For both MADs and TRDs, it’s crucial to consult a dentist who specializes in dental sleep medicine. Proper fitting and regular follow-up are essential to ensure the effectiveness of these devices and to monitor for any potential side effects, such as changes in bite or discomfort. A specialist can customize the appliance to meet your specific needs, ensuring optimal results in managing sleep apnea.
Surgical Options
Uvulopalatopharyngoplasty (UPPP)
Uvulopalatopharyngoplasty (UPPP) is a surgical procedure aimed at reshaping the soft palate to widen the airway. This often involves the removal or reduction of the uvula to prevent it from obstructing airflow during sleep. UPPP is commonly recommended when other treatments, such as CPAP or oral appliances, fail to adequately manage obstructive sleep apnea (OSA).
Tonsillectomy and Adenoidectomy
Tonsillectomy and adenoidectomy are primarily used in children who have enlarged tonsils or adenoids causing OSA. These surgeries involve the removal of the tonsils, adenoids, or both to improve airway function. This approach is particularly effective in pediatric patients, often leading to significant improvement in sleep quality.
Lower Throat Surgeries
Lower throat surgeries target obstructions in the lower pharyngeal region that contribute to OSA. These procedures aim to remove or reduce tissue that blocks the airway, improving airflow and reducing apnea episodes. They are often considered when less invasive treatments are ineffective.
Global Upper Airway Surgeries
Global upper airway surgeries, such as jaw repositioning, are designed to enhance airway function by structurally modifying the upper and lower jaws. These procedures help to tighten soft tissue in the throat, preventing it from collapsing and blocking the airway during sleep. They can be effective for patients with severe anatomical issues contributing to OSA.
Nasal Surgeries
Nasal surgeries are often performed to address structural issues in the nasal cavity that hinder breathing and reduce the effectiveness of PAP or oral appliances. By correcting these nasal obstructions, patients may experience improved airflow and greater success with other sleep apnea treatments.
Hypoglossal Nerve Stimulation (HNS)
HNS Therapy Overview
Hypoglossal Nerve Stimulation (HNS) is a surgical treatment designed to manage obstructive sleep apnea (OSA) by addressing airway blockage through nerve stimulation. This therapy involves implanting a small device that stimulates the hypoglossal nerve, which controls tongue movement. During sleep, the device activates when you inhale, moving the tongue forward to prevent it from collapsing and blocking the airway.
HNS is typically considered a secondary option when positive airway pressure (PAP) therapy fails to provide adequate relief. It offers a targeted approach for patients who do not respond well to other treatments, improving airflow and reducing apnea events.
Lifestyle Changes
Weight Management
Weight management plays a crucial role in managing obstructive sleep apnea (OSA). Studies show that losing weight can significantly reduce the severity of OSA symptoms by decreasing the amount of tissue obstructing the airway. However, sustained weight loss can be challenging due to factors like genetics and lifestyle habits, making it important to approach weight management with a long-term strategy.
Avoiding Alcohol and Sedatives
Alcohol and sedatives can exacerbate OSA symptoms by relaxing the muscles in the throat, leading to more frequent and prolonged airway blockages. Patients with OSA are advised to avoid these substances, especially in the hours before bedtime, to reduce the risk of apnea episodes during sleep. For those who need medication, consulting a doctor for alternatives that don’t worsen OSA is recommended.
Positional Therapy
Positional therapy is another effective lifestyle change for managing OSA. Sleeping on your back can worsen airway obstruction, so avoiding this position can lead to fewer apnea events. Special devices, such as wearable sensors or pillows, can help maintain a side-sleeping position, reducing the risk of airway collapse during sleep.
Exercise
Regular physical activity is beneficial for individuals with OSA, even if it doesn’t lead to significant weight loss. Exercise helps improve overall health and may reduce the severity of OSA by strengthening respiratory muscles and improving oxygen circulation. Incorporating regular exercise into your routine can be an effective part of managing sleep apnea symptoms.
Conclusion
Managing obstructive sleep apnea (OSA) involves a variety of treatment options, from Positive Airway Pressure (PAP) devices and oral appliances to surgical interventions and lifestyle changes. Each option offers unique benefits, but the most effective treatment plan depends on your specific needs and medical history. It’s essential to consult with a healthcare professional, such as an ENT doctor in Singapore, to determine the best course of action.
Taking proactive steps to address OSA is crucial for improving sleep quality and overall health. By exploring the available treatments and seeking expert guidance, individuals with OSA can significantly enhance their well-being and enjoy better, more restful nights.
More information: